GLP-1 is Changing Medicine. Food Quality Matters More Than Ever.
Powerful new drugs amplify one gut satiety signal. Quality food activates the whole system, including a key appetite-regulating system called the ileal brake.
Christopher Damman, Associate Professor of Gastroenterology, School of Medicine, University of Washington. Editor-in-Chief of Gut Bites MD.
GLP-1 has changed the conversation around metabolism. Once a relatively obscure gut hormone, it now seems impossible to open an article about nutrition, weight, or metabolic health without seeing GLP-1 in the headline.
Medications that amplify GLP-1 signaling can meaningfully reduce food intake, lower body weight, and improve the metabolic dysfunction underlying many chronic diseases. For many patients, these medications are a true game changer.
But beneath the headlines sits an important physiological reality. GLP-1 was never meant to work alone.
In normal human biology, GLP-1 is just one component of a coordinated signaling system involving multiple hormones, microbiome signals, and nerve pathways.
If metabolism were an orchestra, GLP-1 would be one important instrument but not the conductor. Food itself coordinates the performance, and food quality still matters even in the era of powerful GLP-1 therapies.
Pharmacology vs Physiology
GLP-1 medications work by producing sustained activation of the GLP-1 receptor at levels the body would not normally generate in the brain, gut, and endocrine organs. This pharmacologic signal suppresses appetite, slows stomach emptying, and improves how our bodies process sugar.
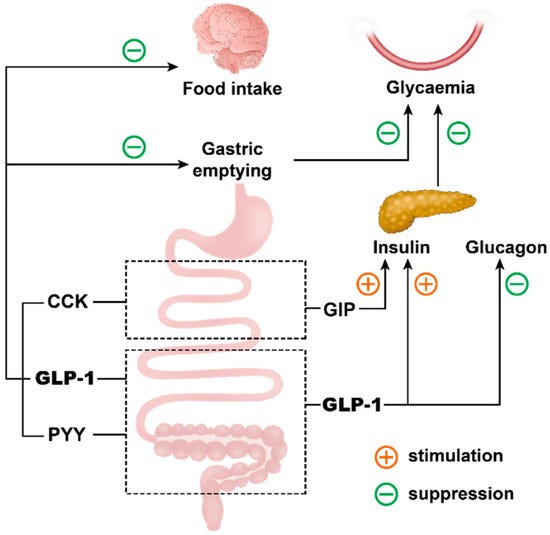
Physiology works differently. After a meal, the intestine releases a cascade of signals including nutrients, factors produced by our microbiome, and a set of gut hormones: GLP-1, GIP, and PYY. Circulating hormone levels are typically far lower than those produced by medications, but the system functions as a coordinated regulatory network rather than a single dominant signal.
Many of these signals act locally within the gut. The vagus nerve, the gut’s information highway, relays this information to the brain, stomach, and other organs. As a result, their effects are not necessarily reflected by generating highest hormone concentrations in the bloodstream. In fact, less processed foods often produce lower GIP and GLP-1 levels in the blood while generating a more coordinated and sustained response within the gut and through vagal signaling.
The Ileal Brake
One of the most important mechanisms in this network is the ileal brake.
When nutrients reach the lower small intestine (the ileum) and colon, they trigger feedback signals that slow stomach emptying and appetite. Specialized cells release hormones such as GLP-1 and PYY that signal through the vagus nerve to the brain. Together these signals slow digestion and help limit further intake.
Rather than producing a high spike in circulating hormones, this system functions as a gradual and subtle braking mechanism that helps regulate appetite over time. How strongly it activates depends largely on what foods reach the lower intestine.
Evidence for the importance of the break comes from weight loss surgery. Gastric bypass leads to more rapid delivery of less-digested nutrients to the lower intestine, strongly activating GLP-1, PYY, and other satiety signals. This enhanced stimulation of the distal gut and improved appetite control is thought to be a key reason these surgeries are so effective for weight loss and metabolic disease.
Food Structure and Composition Determines What Reaches the Brake
Food processing also strongly influences how much intact nutrient material reaches the distal gut, often in the opposite direction.
Minimally processed foods retain structural complexity such as plant cell walls, intact fibers, and resistant starches. These structures slow digestion and allow portions of food to travel further down the intestine before absorption.
Food composition also matters. Components common in less processed foods such as fibers, polyphenols, and unsaturated fats can independently slow digestion and absorption by inhibiting digestive enzymes and slowing glucose absorption.
Highly processed foods often disrupt both structure and composition. Industrial processing breaks down plant structures and concentrates refined carbohydrates and saturated fats while removing fibers, polyphenols, and unsaturated fats. It allows calories to be absorbed rapidly in the upper intestine before the distal gut’s braking signals are fully engaged.
The Microbiome: Fiber and Polyphenols
The microbiome adds another important layer to this system.
Fibers, resistant starches, and many polyphenols escape digestion in the upper gastrointestinal tract and reach the colon, where microbes transform our food’s leftovers into biologically active metabolites.
Fermentation of fiber produces short-chain fatty acids such as butyrate that interact with specialized cells that produce hormones like GLP-1 and neural pathways involved in appetite regulation. Many polyphenols are also transformed into metabolites that influence hormone signaling and inflammation within the gut.
Microbial fermentation therefore acts almost like a slow-release capsule for satiety. While nutrients absorbed earlier in digestion create short-term signals, microbial metabolism provides a longer and steadier signal that helps extend fullness and stabilize appetite. Dietary patterns rich in diverse plant foods tend to strengthen this microbial signaling system.
Food Quality in the Era of GLP-1 Therapy
GLP-1 medications reduce appetite effectively, but they do not automatically determine what foods people choose to eat.
Some studies suggest that individuals using these medications shift modestly toward healthier foods because smaller portions feel more satisfying. Reduced appetite alone, however, does not guarantee adequate protein, micronutrients, or microbiome-supporting foods.
This matters because rapid weight loss without attention to nutrition can contribute to loss of lean muscle mass, nutrient deficiencies, and reduced metabolic resilience. Research supports the important of working with nutrition professionals during GLP-1 therapy so that reduced appetite translates into higher-quality food choices rather than simply lower food intake.
Simple tools that help people measure and score the quality of foods, meals, and recipes can also make this process easier by helping individuals quickly identify whole and better-for-you processed options that support metabolic health.
Principles That Support Physiologic Satiety
Several dietary components consistently support the gut’s natural satiety systems:
Diverse fermentable fibers from intact plant foods
Polyphenol-rich foods such as berries, herbs, spices, tea, coffee, and colorful produce
Whole-food protein paired with fiber and healthy fats
Unsaturated fats from foods such as nuts, seeds, olive oil, and fish
Reduced reliance on ultra-processed foods
These components increase the likelihood that digestion, microbial fermentation, and distal gut signaling work together to regulate appetite.
A Practical Perspective
GLP-1 medications represent an important advance in treating metabolic disease because they can meaningfully reduce appetite and help many patients achieve weight loss that was previously difficult to sustain.
At the same time, the deeper biology of appetite regulation still depends on the interaction between food structure, digestion, microbial metabolism, and gut–brain signaling. Medications can amplify one part of the system, but food still conducts the orchestra.
For that reason, improving food quality and having practical tools to quantify and track that quality in everyday eating remain powerful ways to support metabolic health whether GLP-1 therapy is part of the plan or not.
Christopher Damman, Associate Professor of Gastroenterology, School of Medicine, University of Washington. Editor-in-Chief of Gut Bites MD.





Thank you so much.
Dr Damman,
See our website www.archaealife.com. Polyphenols, digestive enzymes, minerals and other secondary compounds are important to what you talk about.